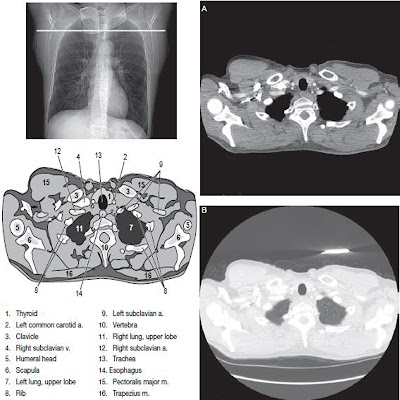
CT Scan of the Liver
The normal CT number attenuation of the liver in unenhanced studies varies among individuals and ranges from 38 to 70 Hounsfield Unit (HU). In healthy patients the attenuation of the liver is at least 10 Hounsfield Unit (HU) greater than that of the spleen.
Fatty Liver CT Studies
Fatty infiltration of the liver is one of the most common abnormalities diagnosed by liver Ct and can result from a variety of causes including:
- Alcoholism
- Obesity
- Diabetes
- Chemotherapy
- Corticosteriod Therapy
- Hyperalimentation – like total parental nutrition-intravenous feeding
- Malnutrition
Fatty infiltration reduces the CT radiation attenuation of the involved liver. With fatty liver infiltration, the liver is at least 10 hounsfield units (HU) lower than that of the spleen. Although it is most commonly a diffuse process, hence the lower attenuation is seen throughout the liver, fatty infiltration can also be focal and differentiate from tumorours mass. Fatty infiltration either diffuse or focal, is most accurately assessed on non-contrast CT scan. Many radiologic technologist include a region of interest (ROI) measurement of the liver and of the spleen. A spleen measurement that is more than 10 hounsfield units (Hu) higher than that of the liver indicated fatty liver infiltration.
 |
| A ROI measurement is placed within the liver and spleen. If the spleen measures 10 HU or more than the liver, fatty infiltrate of the liver is indicated. |
Liver Cavernous Hemangioma
Another common finding in the liver is a cavernous hemangioma. These benign tumors are often discovered incidentally during hepatic imaging by use of ultrasound, CT scan or MRI. Although in the majority of cases hemangioma are solitary, some patients have multiple lesions. Most hemangiomas have a characteristic appearance on CT scan. On non contrast CT scan hemangiomas appear as a well defined hypodense mass of the same density as other blood filled spaces, such as the inferior vena cava. After IV contrast administration the lesion shows progressive pooling of contrast in rounded or oval blood filled spaces at the lesions periphery. In most cases, with further delay the lesion fills in slowly from the periphery, eventually becoming uniformly enhanced. Occasional lesions may not fill in completely, likely because of central thrombosis.
Phases of Enhancement in Liver
Because the liver derives approximately 25% of its blood supply from the hepatic artery and the remaining 75% from the portal vein, there are several phases of enhancement after the intravenous administration of a bolus of contrast material. The first is the hepatic arterial phase typically occurring 15 to 25 seconds after the contrast bolus, followed by the portal venous phase, which begins at 60 to 70 seconds after contrast injection. Based on contrast circulation, the hepatic arterial phase can be further divided. The equilibrium phase, sometimes called the late or delayed phase, occurs several minutes after injection.
For routine abdominal CT or as part of a chest, abdominal and Pelvic CT study, the liver is most often scanned just one, during the portal venous phase. However, for some indications scanning in more than one enhancement phase may improve the examination’s sensitivity. Some tumors are supplied by an abnormal number of external blood vessels like hypervascular tumors. Because of this increased blood supply these tumors will display more intense enhancement after an intravenous contrast administration. These are often described as hyperenhancing relative to surrounding liver tissue are best detected during the late arterial phase. Liver metastases tend to be hypervascular in cases of primary tumors of the thyroid or pancreatic islet cells, carcinoid tumors, renal cell carcinoma, some breast tumors and melanoma. When these are suspected, dual phase imaging is often beneficial. However, the majority of liver matastases are hypovascular and develop from primary tumors of the colon and rectum, pancreas, lung urothelium, prostate and most gynecologic images are typically acquired in a single portal venous phase.







1 comment:
While I agree for nationalization of the healthcare services, the root cause is that we have limited the number of doctors that we produce in our country.best liver transplant hospital in indiabest liver transplant hospital in india
Post a Comment